Meet the Device that is Leading AI Skin Cancer Detection
Using AI-driven technology, the DermaSensor device is an FDA cleared, non-invasive solution for skin cancer detection.
The device helps speed up the detection of suspicious lesions at the point of care.
- Detect 3 top skin cancers with 96% sensitivity*
- FDA-cleared results in seconds
- Reimbursement assistance available now
*Clinical evidence upon request
As Featured In














Enhance Your Clinical Confidence in Skin Cancer Detection
Early detection is crucial. Yet traditional visual assessment is entirely subjective and highly variable. DermaSensor helps you assess cancerous lesions with speed and confidence and has been shown to result in more timely referrals to dermatology and improve peace of mind.*
Clinical Highlights:
- Detect 3 top skin cancers with 96% sensitivity*
- FDA-cleared results in seconds
- Reimbursement assistance available now
*Clinical evidence upon request
Intuitive Three-Step Process From First Recording to the Result in 30 Seconds
Step 1
Identify lesion suggestive of skin cancer on the patient.
Step 2
Apply the handheld DermaSensor device to the lesion and initiate first recording. A total of five spectral recordings are taken from the skin lesion to complete the scan.
Step 3
DermaSensor’s algorithm analyzes spectral data and delivers skin cancer risk results in seconds.
Learn more about How DermaSensor works in real clinical settings here
Ready to implement?

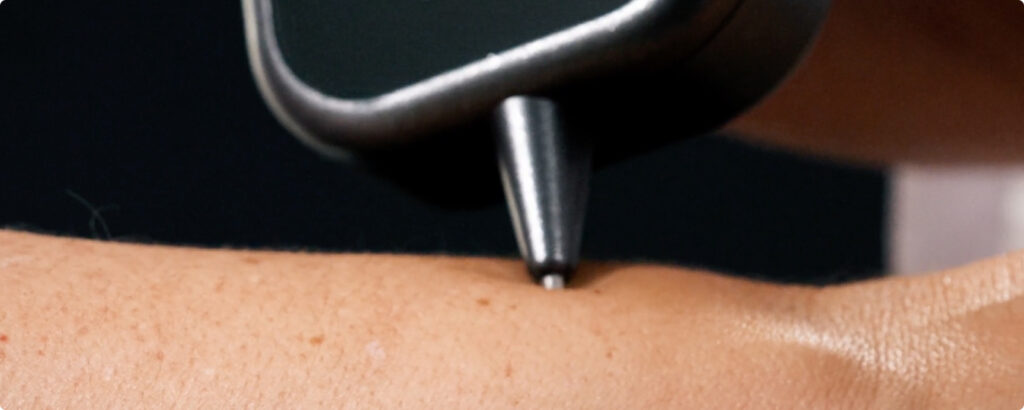

Advanced AI and Optical Spectroscopy in the Palm of Your Hand
Proven Clinical Utility
The DermaSensor device uses a combination of cutting-edge optical spectroscopy and artificial intelligence to promptly analyze suspicious skin lesions. Our proprietary algorithms, developed and refined over a decade of clinical research, are trained on thousands of diagnosed lesions to help you make better informed decisions.
15 development, validation, and clinical utility studies to date with 5,000 lesions scanned and diagnosed*
DermaSensor’s™ tip reflects and records quick bursts of light off the lesion’s cellular and sub-cellular content.
The light is analyzed by the built-in computer to provide information to help physicians assess skin lesions (including melanomas, squamous cell carcinomas, and basal cell carcinomas) to aid in a
referral decision.
By examining the difference in light scattering, DermaSensor™ provides an immediate “Investigate Further” or
“Monitor,” output based on the lesion’s malignancy risk level.
Elastic Scattering Spectroscopy (ESS) has been validated in 30+ publications on clinical studies in various tissue types.Many studies have shown that ESS provides information that is comparable to histopathologic assessment in the analysis of cellular microscopic structure.
HCPs Who Use DermaSensor?
Widely used across multiple healthcare specialties, DermaSensor fits seamlessly into practices of all types—concierge practice, family medicine, internal medicine, and large health systems, among others. Join the growing network of physicians who are enhancing their practices.
Family Medicine

“Yes, I would recommend it. I don’t think physicians (non-derm) learn enough about abnormalities resulting in increased referrals.The device can be used as a guide and the patient will be happier”
Dr. Goisse
Montgomery Medical
Internal Medicine

“I am excited to offer this new technology for skin cancer detection to the patients in my primary care office. The 4-6 month wait time to get in with a dermatologist in our area creates much anxiety.”
Dr. Josephine Lake
Lake Internal Medicine
Concierge Practice

“As a plastic surgeon, this has been fantastic because if I have been somewhat on the fence about a particular skin lesion and I’m not sure, this can give me some more added security and it gives me more data and allows me to dig deeper into a particular skin lesion.”
Alex Zuriarrain, MD, FACS
Hydrology Wellness
Health Systems

“By integrating this technology into our resident training program, the Florida State University Family Medicine Residency Program at BayCare Health System aims to empower its future physicians with enhanced skin cancer detection skills and the ability to provide the best possible care to their patients.”
Dr. Nathan Falk
Professor. Founding Program Director at Family Medicine Residency at BayCare Health System
Walk-in Clinic

Dermasensor’s breakthrough AI technology streamlines skin cancer detection services at the point of care.

“Yes, I would recommend it. I don’t think physicians (non-derm) learn enough about abnormalities resulting in increased referrals.The device can be used as a guide and the patient will be happier”
Dr. Goisse
Montgomery Medical

“I am excited to offer this new technology for skin cancer detection to the patients in my primary care office. The 4-6 month wait time to get in with a dermatologist in our area creates much anxiety.”
Dr. Josephine Lake
Lake Internal Medicine

“As a plastic surgeon, this has been fantastic because if I have been somewhat on the fence about a particular skin lesion and I’m not sure, this can give me some more added security and it gives me more data and allows me to dig deeper into a particular skin lesion.”
Alex Zuriarrain, MD, FACS
Hydrology Wellness

“By integrating this technology into our resident training program, the Florida State University Family Medicine Residency Program at BayCare Health System aims to empower its future physicians with enhanced skin cancer detection skills and the ability to provide the best possible care to their patients.”
Dr. Nathan Falk
Professor. Founding Program Director at Family Medicine Residency at BayCare Health System

Dermasensor’s breakthrough AI technology streamlines skin cancer detection services at the point of care.
Real Results, Real Stories
“I think this is a revolutionary new product that can help us aid in the management of safety and wellness for our patients. In that, we can highlight and see whether any areas, dark areas, could potentially be cancerous.”
Dr. Anthony Ceccacci, Madison Avenue Aesthetics
“Integrating DermaSensor’s innovative technology into our practice, we now offer enhanced skin cancer assessment capabilities in our community, ensuring timely referrals for our patients.”
Dr. Kevin Wong, Founder of PT Family Medicine
“If you have DermaSensor, in 15 or 30 seconds, you can advise your patient that this is something you are going to refer to a dermatologist, or keep an eye on it, and you can re-evaluate on their next visit.”
Dr. Paul Hart, Physician
“I mean, a lot of my patients are very complex. It’s like an internal medicine practice.
You just had to, you just have to get it into your brain that it’s available.”
Dr. Marcy Gooise, Montgomery Medical
“For me, it was a no-brainer to choose the device…it’s crucial to recognize that skin cancers do not always present the same way in people of color.”
Dr. Jessica Shepherd, MD, MBA, FACOG Renowned Gynecologist and Good Morning America Media Personality
“The beauty of the device is how simple it is… it is simple, easy, and straightforward.”
Dr. Brian Hollett, SHIFT | Concierge Primary Care in Chicago CMO
“The feedback from patients has been excellent…giving them peace of mind about their skin cancer risk.”
See How Derma Sensor
Fits Your Practice

New Reimbursement Assistance Now Available for DermaSensor
Getting reimbursed for innovative care should be simple. That’s why we’re excited to announce that DermaSensor now offers reimbursement guidance, at no cost to you and your patients, through our partnership with TRG (The Reimbursement Group). Speak to a consultant today to learn more about this reimbursement support and the introductory pricing offers for the DermaSensor device.
What You Will Receive from TRG (The Reimbursement Group) If You Are a DermaSensor Customer:
- Targeted Support: Assistance tailored to the patient’s payer requirements
- Documentation Help: Guidance Information to support the preparation of documentation for government and private insurance plans to support coverage and payment
- Download the latest Coding Guide
Need help? It’s easy.
Call (888) 298-8848
Learn More About DermaSensor's 3-Month Introductory Device Offer.
Major FDA Cleared Product Firsts:
- First skin cancer device developed for PCPs
- First FDA Breakthrough device for skin cancer
- First automated device indicated for all three common skin cancers (Melanoma, BCC and SCC)
- Only skin cancer device available that provides any risk assessment using any type of imaging or optical technology
What’s Included
Experience AI-powered skin cancer detection for 90 days. Expert support. Risk-free.
Charging dock, power supply, and regional power adapter blades.
Software updates directly to your DermaSensor.
Free access to courses for you and your employees. Accessories Included: Charging dock, power supply, and regional power adapter blades.
Helps elevate your practice: Unlock new patient opportunities by joining the physician finder!
If you have any questions regarding DermaSensor, our support team is here to help.
Customers can manage their devices to see the cloud backups.
Monitors connectivity an dutilization.
Spot it First.
Stay Informed
Never miss important updates. Subscribe to receive news, events,
and documents straight to your inbox.
Take the Next Step
Advance Your Practice with AI-Powered Skin Cancer Detection in the Palm of your Hand!
